How do you, RESPECT our elder’s wishes of, DNR, this is, difficult, because, if we do, then, we would carry the names of, being, cruel, as children, but if we don’t, we’re, equally, unfitting, so, this is, very hard, to, do…from the files of a nephrologist, translated…
With the Many Medical Advancements of Today, being a Medical Professional, I’d Often Seen that the Patients, Getting to the Terminal Stages of Their, Lives, with No Chances, while Their Families Still Wanted Us to Try and Save Their, Lives………
We can’t choose when we were, born, but can we, choose when we would, die? As we get to the, end, would our own decisions be, altered, by our families’, “kindness”, or, will the ones we loved, although unwilling to let us go, but still, chose to, respect our, wishes?
Finding that Balance Between the Patients’ Will & the Medical Treatment, Means
My mother’s ninety-five this year, with four generations of, offspring, and we’re all, around her, her life is happy, it’s what most envied. But with the coming of her, years, her system started, malfunctioning, her long-term diabetes, with the combined kidney disease, the loss of her muscles, causing her to start, deteriorating, away. Last year, she was hospitalized because of an infected wound, for almost, a whole, week. At the beginning of this year, he was diagnosed with her breast cancer which had, come back, again, but, the unpleasant experience of her hospitalization last year, getting her shots every single day, it’d caused her to reject the hospitalizations. Sometimes, we would see her, use her scarf, wrapped it around her neck, and she’d looked like she wanted to, hang herself, and we’d asked her why, she’d not wanted to, burden us anymore, and this made us all feel, awful.
illustration from UDN.com

Since the start of the year, when Lien-Jing’s mother had contracted CoVid-19, she’d become, bedridden most of her time now. at the end of February, we’d found her to sleep for the entire day, reduced her food intakes, as I’d heard, I’d worried that she may have the electrolyte imbalance, or the lowering of the immunities, which will cause her to become, easily, infected, I’d suggested to the family to take her to the hospitals, to check, and to get her the proper, treatments. But, Lien-Jing’s whole family, decided to follow their mother’s wishes, only kept her at home, and, fed her small amounts of liquids, the rice soups, the milk.
One day, the elderly fell into, a coma, they’d notified the daughter who is in the U.S. to come home quick, and prepared for the clothes for her final passage. I’d gone to visit, found that she was breathing evenly, that she had normal circulation of her lower extremities, that she can be, treatable, so I’d, talked it over with Lien-Jing. And yet, considering the elder’s wishes, in the end, they’d still decided to keep her at home, with NO invasive treatment, measures being performed.
Several days later, Lien-Jing’s mother’s health seemed to be in a stasis, after discussing it with the local medical systems providers, the medical teams were willing to go to her home, to put her on the drips, to get her enough nutrients, electrolytes too, the physicians also made the scheduled visits. And so, in not going against the elder’s wishes both sides found a way that, worked.
Who is it For, What the Patients are Weathering, in Their, Terminal, Stages of, Life?
As hard as it is, this family still, NEVER went against the elder’s wishes, kept her at home, to care for her. They’d stayed by the elder twenty-four hours a day, and, whether it be flipping the elder over, feeding her, massaging her body, baths in bed, the members of the families, did themselves. When I saw Lien-Jing by his mother’s bed, holding his mother’s hand, calling out to her, telling her everything they’d gone through, together, hoping that with his voice, he could, somehow, wake his mother, up again, I was, truly, moved by him.
A month passed, the elderly slowly became, awake, and could start eating on her, own, and could, recall the past with Lien-Jing too. It’s just, that she’d mentioned to her daughter, “I don’t want to live anymore”.
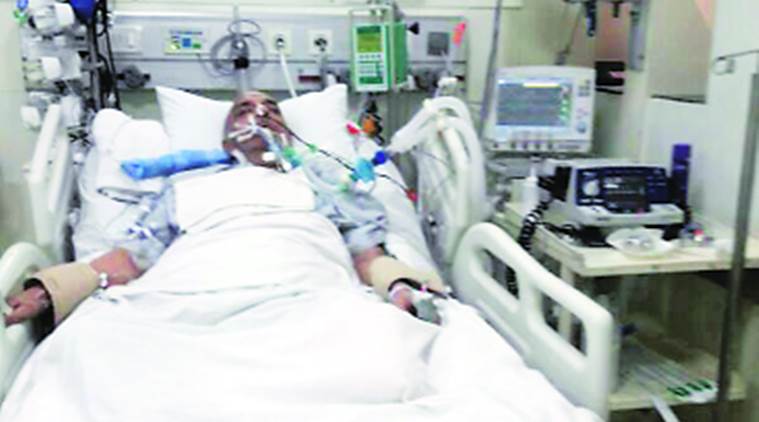
With the medical advancements being available to all, as a physician, I’d often seen the patients, getting to their, terminal stages of life, with the families, desperately, trying to, get them, back to life. And in the end, the patients were connected to the tubes, with the ulcers inside their, oral, cavities, edema, the hands and feet, turning, black…………toward this, I can’t help, but wonder: is the terminal treatments in one’s life, for oneself only, or, is it, for the, benefit of, the loved, ones?

would you want your loved ones to live out the rest of her/his life, like this??? Photo from online
In after seeing a ton of the offspring, with the names of filial piety, putting their elders through the unnecessary tortures, turning “patients’ will” into, an, illusion, I’d become, totally in awe of Lien-Jing and her families’ way of handling her mother’s, final, passage: allowing her mother to decide how she wanted to, die.
And so, this, is on being caught between being, unfitting as the offspring, or, to let our loved ones, stop, suffering, and unfortunately, in these Asian society, we’re all, too often, kidnapped by the beliefs of, filial piety, and, we put our elderly loved ones, through the hells that they don’t, deserve but gladly, this family, didn’t.










You must be logged in to post a comment.